September 2021
Top 5 Causes of Swollen Feet
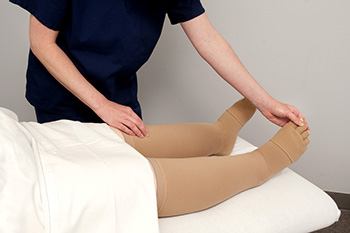
There are many possible causes of swollen feet—ranging from mild, temporary conditions to severe medical emergencies. Here is a run-down of the top 5: 1) Trauma. After an injury, the body’s inflammatory response floods the injured area with white blood cells, antibodies, proteins, and other fluids, causing swelling and inflammation. 2) Diseases. Diseases of the heart, kidney, liver, and lymphatic system can compromise the body’s ability to pump or regulate the blood, and expel wastes, causing a build-up of fluid in various parts of the body—including the feet and legs. 3) Venous Insufficiency. Swelling in the feet and legs may occur when the venous valves—which return blood back to the heart—are damaged and dysfunctional. 4) Pregnancy. Hormonal surges and a growing uterus pressurize veins and increase water and sodium—leading to edema (swelling) in the feet, hands, and legs. 5) Inactivity. Sitting or standing still for prolonged periods of time can cause fluid to temporarily accumulate in the tissues of the feet and ankles. If your feet or ankles become swollen or painful, schedule an appointment with a podiatrist.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Mark Spier from Maryland. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact one of our offices located in Columbia and Reisterstown, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
Should I See a Doctor for My Heel Pain?
 Heel pain is one of the most common conditions podiatrists help treat, and it can have a variety of causes. Common causes of heel pain include plantar fasciitis, Achilles tendonitis, bursitis, a ruptured Achilles tendon, or a heel fracture. There are a few key signs that your heel pain may be serious and needs to be checked by a podiatrist. If the pain continually worsens, stops you from doing daily activities, has not improved after a couple of weeks, or causes a tingling sensation in the heel, there may be a more serious issue at play that should be checked by a podiatrist. If the pain is severe, hinders your ability to walk, or was accompanied by a popping sensation at the time of injury, these may be signs of an even more serious injury that should be treated immediately.
Heel pain is one of the most common conditions podiatrists help treat, and it can have a variety of causes. Common causes of heel pain include plantar fasciitis, Achilles tendonitis, bursitis, a ruptured Achilles tendon, or a heel fracture. There are a few key signs that your heel pain may be serious and needs to be checked by a podiatrist. If the pain continually worsens, stops you from doing daily activities, has not improved after a couple of weeks, or causes a tingling sensation in the heel, there may be a more serious issue at play that should be checked by a podiatrist. If the pain is severe, hinders your ability to walk, or was accompanied by a popping sensation at the time of injury, these may be signs of an even more serious injury that should be treated immediately.
Many people suffer from bouts of heel pain. For more information, contact Dr. Mark Spier of Maryland. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact one of our offices located in Columbia and Reisterstown, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Six Ways to Treat Diabetic Foot Ulcers
Diabetic foot ulcers (DFUs) are wounds that occur on the feet of diabetic patients. These wounds may heal poorly, slowly, and have an increased risk of becoming infected. Because of this, prompt and proper wound care is necessary. Your podiatrist may treat your DFU by keeping pressure off of the wound using casts, boots, specialty shoes, or off-loading devices. The wound may also need to be debrided, which involves removing dead or damaged tissue and any foreign objects from the wound. You will then need to keep the foot clean and dry and moisturize the area with a prescribed cream to promote healing. Your doctor might also suggest ways to improve your circulation or prescribe additional therapies to encourage the wound to heal. For more information about caring for DFUs, please consult with a podiatrist.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Mark Spier from Maryland. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
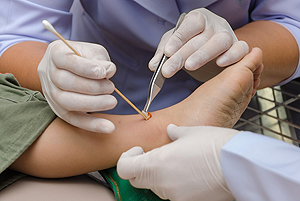
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Columbia and Reisterstown, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Do Your Child's Feet Hurt?
What to Know About a Broken Toe
The forefoot is composed of five metatarsal bones and fourteen phalanges. Each toe has three phalanges except for the big toe which only has two. Our toes play an essential role to the walking process, which is why a broken toe could seriously disrupt one’s ability to move around. Toe fractures are common and can be very painful. Fortunately, these injuries rarely require surgery and usually heal with rest and a change in activity.
Broken toes typically result from a traumatic event such as falling, stubbing the toe, or dropping something on the toe. Traumatic toe fractures may be categorized as either minor or severe fractures. At times, one may hear a “pop” or “crack” sound when the bone breaks. Common symptoms of a traumatic toe fracture include pain, throbbing, bruising, swelling, and redness.
Another type of toe fractures is a stress fracture. These injuries usually appear in the form of small hairline breaks on the bone. Stress fractures develop after repetitive activity instead of a single injury. Stress fractures occur when the muscles in the bone become too weak to absorb impact. Consequently, the toe bone becomes vulnerable to any pressure and impact it endures. Symptoms for a stress fracture in the toe include swelling without bruising, tenderness to the touch, pain that goes away with rest, and pain after walking or running.
If you suspect that you have a broken toe, you should make an appointment with your podiatrist. He or she will likely diagnose you by performing a physical exam and an X-ray. Treatment for a broken toe may include the R.I.C.E. method, buddy taping, surgery, or antibiotics. The R.I.C.E. method (Rest, Ice, Compression, and Elevation) is a common treatment method for many injuries because it decreases pain. Buddy tapping involves wrapping the injured toe next to an adjacent toe to keep it supported and protected. These two methods have proven to be effective in the healing process for toe fractures. The estimated healing time for a broken toe is approximately four to six weeks. If the injury becomes infected or requires surgery, the estimated healing time may take eight weeks or more.
Fracture of the Pinky Toe
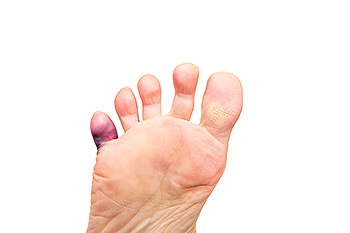 The pinky toe is the smallest toe on the foot, and it is located on the outside of the foot. It can easily be involved in an injury and be painful to deal with when broken. A broken pinky toe will often appear to be bruised, and can turn red and purple. Some patients experience swelling, as well as misalignment of the affected toe. An effective diagnosis may involve undergoing an X-ray, which can help to determine what type of fracture it is. A hairline fracture can be treated by resting the affected foot, and relief may be found when an elastic bandage is worn. Patients who are over sixty-five may be prone to enduring a dislocated toe, meaning separation of the bones in the toe. If you feel you may have broken your toe, it is strongly suggested that you are under the care of a podiatrist who can help you with correct treatment options.
The pinky toe is the smallest toe on the foot, and it is located on the outside of the foot. It can easily be involved in an injury and be painful to deal with when broken. A broken pinky toe will often appear to be bruised, and can turn red and purple. Some patients experience swelling, as well as misalignment of the affected toe. An effective diagnosis may involve undergoing an X-ray, which can help to determine what type of fracture it is. A hairline fracture can be treated by resting the affected foot, and relief may be found when an elastic bandage is worn. Patients who are over sixty-five may be prone to enduring a dislocated toe, meaning separation of the bones in the toe. If you feel you may have broken your toe, it is strongly suggested that you are under the care of a podiatrist who can help you with correct treatment options.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact Dr. Mark Spier from Maryland. Our doctor will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
- Swelling
- Pain (with/without wearing shoes)
- Stiffness
- Nail Injury
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions, please feel free to contact one of our offices located in Columbia and Reisterstown, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.